Prof. N. Reha Tandoğan, M.D. - Asım Kayaalp, M.D.
What is a partial (unicondylar) knee arthroplasty?
A partial knee arthroplasty is the surface replacement of only the diseased compartment of the knee. Typically more common on the inner (medial) side of the knee, the diseased cartilage and the underlying bone is covered with metal and polyethylene implants. (Figure 1).Figure 1a,b: Comparison of a total and partial knee replacement.
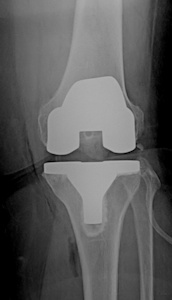
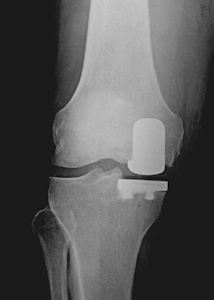
The implants are made of metal femoral and tibial components with a plastic (polyethylene) insert between the articulating surfaces. The surgeon can choose between a fixed and mobile bearing design depending on his experience and preference (Figure 2). Medial and lateral implants are available for the replacement of inner and outer side of the knee.
Figure 2a,b: Mobile & fixed bearing unicondylar implants


Who would benefit from a partial knee replacement?
A partial knee replacement is suitable for patients with joint degeneration confined to a single compartment of the knee. The patient should preferably be older than 60 years of age, however unicondylar knee replacement can safely be performed in patients in their fifties if other treatment alternatives have failed. The pain should be localized to the involved compartment, patients with widespread pain in the knee have a low chance of benefit from a partial knee arthroplasty. The damage in the joint should be localized to a single compartment and the rest of the joint cartilage, menisci and ligaments should be normal. The deformity of the knee should be correctable during examination. Unicondylar knee replacement is not suitable for patients with cartilage damage involving more than one compartment, and in patients with inflammatory arthritis (such as rheumatoid arthritis and ankylosing spondylitis). Osteonecrosis is a disease where the blood vessels to a small area in the bone become clogged, resulting in bone death and collapse of the weakened area. This area is surrounded by normal bone and cartilage. Partial knee replacement is suitable for patients with localized osteonecrosis (Figure 3). When all of the above criteria are met, unicondylar knee replacement may be suitable for 15% of the patients with knee osteoarthritis.Figure 3a,b: Partial knee replacement in a patient with osteonecrosis of the medial femoral condyle.
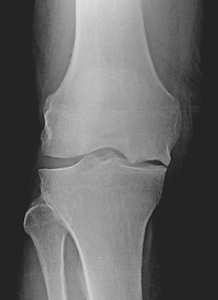
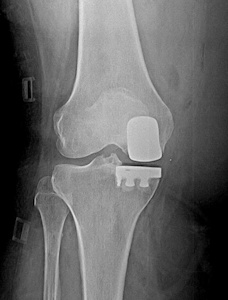
What are the advantages of a partial knee replacement?
Compared to total knee replacement, partial knee replacements have several advantages- The recovery period is quicker and less painful. Restoration of knee range of motion and muscle strength takes a shorter period of time. This is possible due to the small incisions and avoiding damage to the uninvolved structures. Hospitalization is around 3 days for a total knee and 2 days for a partial knee replacement. Most patients with partial knees do not require a formal physiotherapy program and can be safely managed with a home rehab program and self exercises.
- The feeling of a “normal joint” or a “forgotten joint” is higher in patients with partial knees. A forgotten joint is the situation where the patient has no pain or limitation in activities of daily living and essentially forgets the joint that has been operated. The reason for this is the preservation of menisci, ligaments and bone in the uninvolved knee, thus preserving the deep sensation nerves and restoration of normal knee kinematics.
- The surgery is performed through smaller incisions, resulting in a smaller scar.
- The activity level after a partial knee replacement is higher than a total knee. Most active patients can perform low impact sports such as hiking, cycling and swimming. Doubles tennis is possible. However it should be noted high impact activities involving running and jumping are detrimental for the longevity of the implant and should be avoided.
Are partial knee replacements durable?
Previous designs of partial knee replacements had high failure rates due to inferior pain control, early wear and loosening. Modern implant designs, better patient selection and advances in surgical techniques have led to dramatic improvements in the outcomes of partial knee replacements. Current partial knee implants have a survival rate of over 90% at ten years. This rate becomes 75-80% at 15 to 20 years. The outcome of partial knee replacement is dependent on many factors including the implant, surgical technique and patient selection. The experience of the surgeon has also been shown to be important for a good outcome and implant survival. Studies have shown that, the more number of surgeries performed by the surgeon, the better the results.Is partial knee replacement suitable for me?
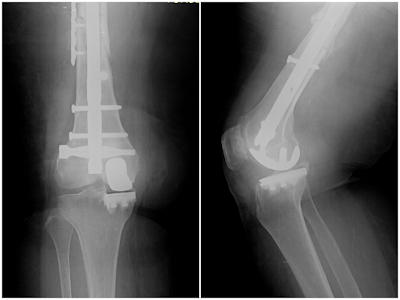
Your surgeon will first examine your knee, evaluate your X-rays and order a magnetic resonance imaging study if needed. He will discuss the advantages and drawbacks of a partial knee replacement. Although the preoperative work-up gives strong clues about the suitability of a partial knee replacement, the final decision will be made during surgery when your doctor sees the condition of your knee. Very rarely, your surgeon might decide to perform a total knee replacement if the damage in your knee is more severe than anticipated before surgery. Partial knee replacement is an excellent option in select patients with implants in the femur that cannot be removed (Figure 4)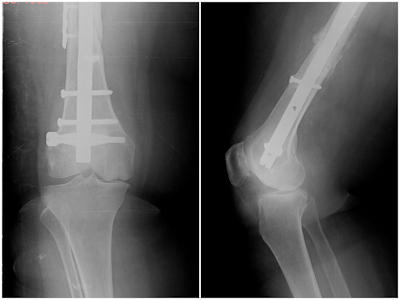
What kind of activities can I do after a partial knee replacement?
Activities of daily living such as walking, cycling, going up and down the stairs, and kneeling are possible after a partial knee replacement. There are no restrictions on driving after the first month of surgery. Swimming, golf, jogging and bowling are permitted. Sports involving running, jumping and cutting movements such as soccer, basketball, singles tennis, and volleyball are not advised. Patient who are good skiers before knee replacement can ski on gentle slopes with in low speeds. Impact sports are not permitted as these activities might cause early wear and loosening of the implant leading to failure.What are the risks of partial knee replacement?
The most important failure reason of a partial knee replacement is disease progression in the un-resurfaced parts of the knee. When this happens, a total knee replacement might be needed to regain function. This problem is seen in 10-15% of the patients and increases with longer term follow-up. Another way of looking at this is that, a partial knee replacement can delay the need for a total knee implant for 10-15 years in select patients. Conversion to a total knee replacement is not technically challenging and the outcomes are no different from a primary total knee replacement.Spinning out of the mobile plastic insert may be seen in 2-4% of the cases with mobile bearing implants. These are mostly due to technical errors. Wear of the plastic may occur in fixed bearing implants, however is rare before 10 years with modern implants.
All materials permanently implanted into the body carry a risk if infection. Early infections may be treated with surgical cleaning (irrigation) and changing the plastic insert; metal parts of the implant may be retained. Late infections (occurring more than 6weeks after implantation) may require removal of the implant, placement of an antibiotic spacer and conversion to a total knee replacement in the second stage. The risk of infection after a partial knee is less than 1% in most patients. This rate may be higher in high risk patients with accompanying severe medial diseases.
Migration of the implant is sinking of the implant into soft bone causing failure. Fractures may occur during surgery or after a fall. Fortunately these are very rare.
